Celiac Disease
What is celiac disease?
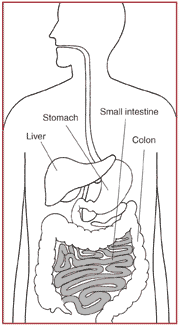
Celiac disease is a digestive disease that damages the small intestine and interferes with absorption of nutrients from food. People who have celiac disease cannot tolerate a protein called gluten, found in wheat, rye, and barley. Gluten is found mainly in foods but may also be found in products we use every day, such as stamp and envelope adhesive, medicines, and vitamins.
The small intestine is shaded above.
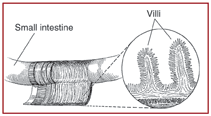
When people with celiac disease eat foods or use products containing gluten, their immune system responds by damaging the small intestine. The tiny, fingerlike protrusions lining the small intestine are damaged or destroyed. Called villi, they normally allow nutrients from food to be absorbed into the bloodstream. Without healthy villi, a person becomes malnourished, regardless of the quantity of food eaten.
Villi on the lining of the small intestine help absorb nutrients.
Because the body’s own immune system causes the damage, celiac disease is considered an autoimmune disorder. However, it is also classified as a disease of malabsorption because nutrients are not absorbed. Celiac disease is also known as celiac sprue, nontropical sprue, and gluten-sensitive enteropathy.
Celiac disease is a genetic disease, meaning it runs in families. Sometimes the disease is triggered—or becomes active for the first time—after surgery, pregnancy, childbirth, viral infection, or severe emotional stress.
What are the symptoms of celiac disease?
Celiac disease affects people differently. Symptoms may occur in the digestive system, or in other parts of the body. For example, one person might have diarrhea and abdominal pain, while another person may be irritable or depressed. In fact, irritability is one of the most common symptoms in children.
Symptoms of celiac disease may include one or more of the following:
- gas
- recurring abdominal bloating and pain
- chronic diarrhea
- constipation
- pale, foul-smelling, or fatty stool
- weight loss/weight gain
- fatigue
- unexplained anemia (a low count of red blood cells causing fatigue)
- bone or joint pain
- osteoporosis, osteopenia
- behavioral changes
- tingling numbness in the legs (from nerve damage)
- muscle cramps
- seizures
- missed menstrual periods (often because of excessive weight loss)
- infertility, recurrent miscarriage
- delayed growth
- failure to thrive in infants
- pale sores inside the mouth, called aphthous ulcers
- tooth discoloration or loss of enamel
- itchy skin rash called dermatitis herpetiformis
A person with celiac disease may have no symptoms. People without symptoms are still at risk for the complications of celiac disease, including malnutrition. The longer a person goes undiagnosed and untreated, the greater the chance of developing malnutrition and other complications. Anemia, delayed growth, and weight loss are signs of malnutrition: The body is just not getting enough nutrients. Malnutrition is a serious problem for children because they need adequate nutrition to develop properly. (See Complications.)
Why are celiac disease symptoms so varied?
Researchers are studying the reasons celiac disease affects people differently. Some people develop symptoms as children, others as adults. Some people with celiac disease may not have symptoms, while others may not know their symptoms are from celiac disease. The undamaged part of their small intestine may not be able to absorb enough nutrients to prevent symptoms.
The length of time a person is breastfed, the age a person started eating gluten-containing foods, and the amount of gluten-containing foods one eats are three factors thought to play a role in when and how celiac disease appears. Some studies have shown, for example, that the longer a person was breastfed, the later the symptoms of celiac disease appear and the more uncommon the symptoms.
How is celiac disease diagnosed?
Recognizing celiac disease can be difficult because some of its symptoms are similar to those of other diseases. In fact, sometimes celiac disease is confused with irritable bowel syndrome, iron-deficiency anemia caused by menstrual blood loss, Crohn’s disease, diverticulitis, intestinal infections, and chronic fatigue syndrome. As a result, celiac disease is commonly underdiagnosed or misdiagnosed.
Recently, researchers discovered that people with celiac disease have higher than normal levels of certain autoantibodies in their blood. Antibodies are protective proteins produced by the immune system in response to substances that the body perceives to be threatening. Autoantibodies are proteins that react against the body’s own molecules or tissues. To diagnose celiac disease, physicians will usually test blood to measure levels of
- Immunoglobulin A (IgA)
- anti-tissue transglutaminase (tTGA)
- IgA anti-endomysium antibodies (AEA)
Before being tested, one should continue to eat a regular diet that includes foods with gluten, such as breads and pastas. If a person stops eating foods with gluten before being tested, the results may be negative for celiac disease even if celiac disease is actually present.
If the tests and symptoms suggest celiac disease, the doctor will perform a small bowel biopsy. During the biopsy, the doctor removes a tiny piece of tissue from the small intestine to check for damage to the villi. To obtain the tissue sample, the doctor eases a long, thin tube called an endoscope through the mouth and stomach into the small intestine. Using instruments passed through the endoscope, the doctor then takes the sample.
Screening
Screening for celiac disease involves testing for the presence of antibodies in the blood in people without symptoms. Americans are not routinely screened for celiac disease. Testing for celiac-related antibodies in children less than 5 years old may not be reliable. However, since celiac disease is hereditary, family members, particularly first-degree relatives—meaning parents, siblings, or children of people who have been diagnosed—may wish to be tested for the disease. About 5 to 15 percent of an affected person’s first-degree relatives will also have the disease. About 3 to 8 percent of people with type 1 diabetes will have biopsy-confirmed celiac disease, and 5 to 10 percent of people with Down syndrome will be diagnosed with celiac disease.
What is the treatment?
The only treatment for celiac disease is to follow a gluten-free diet. When a person is first diagnosed with celiac disease, the doctor usually will ask the person to work with a dietitian on a gluten-free diet plan. A dietitian is a health care professional who specializes in food and nutrition. Someone with celiac disease can learn from a dietitian how to read ingredient lists and identify foods that contain gluten in order to make informed decisions at the grocery store and when eating out.
For most people, following this diet will stop symptoms, heal existing intestinal damage, and prevent further damage. Improvements begin within days of starting the diet. The small intestine is usually completely healed in 3 to 6 months in children and younger adults and within 2 years for older adults. Healed means a person now has villi that can absorb nutrients from food into the bloodstream.
In order to stay well, people with celiac disease must avoid gluten for the rest of their lives. Eating any gluten, no matter how small an amount, can damage the small intestine. The damage will occur in anyone with the disease, including people without noticeable symptoms. Depending on a person’s age at diagnosis, some problems will not improve, such as delayed growth and tooth discoloration.
Some people with celiac disease show no improvement on the gluten-free diet. This condition is called unresponsive celiac disease. The most common reason for poor response is that small amounts of gluten are still present in the diet. Advice from a dietitian who is skilled in educating patients about the gluten-free diet is essential to achieve the best results.
Rarely, the intestinal injury will continue despite a strictly gluten-free diet. People in this situation have severely damaged intestines that cannot heal. Because their intestines are not absorbing enough nutrients, they may need to receive nutrients directly into their bloodstream through a vein, or intravenously. People with this condition may need to be evaluated for complications of the disease. Researchers are now evaluating drug treatments for unresponsive celiac disease.
| The web contains information about celiac disease, some of which is not accurate. The best people for advice about diagnosing and treating celiac disease are one’s doctor and dietitian. |
The Gluten-free Diet
A gluten-free diet means not eating foods that contain wheat (including spelt, triticale, and kamut), rye, and barley. The foods and products made from these grains are also not allowed. In other words, a person with celiac disease should not eat most grain, pasta, cereal, and many processed foods. Despite these restrictions, people with celiac disease can eat a well-balanced diet with a variety of foods, including gluten-free bread and pasta. For example, people with celiac disease can use potato, rice, soy, amaranth, quinoa, buckwheat, or bean flour instead of wheat flour. They can buy gluten-free bread, pasta, and other products from stores that carry organic foods, or order products from special food companies. Gluten-free products are increasingly available from regular stores.
Checking labels for “gluten free” is important since many corn and rice products are produced in factories that also manufacture wheat products. Hidden sources of gluten include additives such as modified food starch, preservatives, and stabilizers. Wheat and wheat products are often used as thickeners, stabilizers, and texture enhancers in foods.
“Plain” meat, fish, rice, fruits, and vegetables do not contain gluten, so people with celiac disease can eat as much of these foods as they like. Recommending that people with celiac disease avoid oats is controversial because some people have been able to eat oats without having symptoms. Scientists are currently studying whether people with celiac disease can tolerate oats. Until the studies are complete, people with celiac disease should follow their physician’s or dietitian’s advice about eating oats. Examples of foods that are safe to eat and those that are not are provided in the table below.
The gluten-free diet is challenging. It requires a completely new approach to eating that affects a person’s entire life. Newly diagnosed people and their families may find support groups to be particularly helpful as they learn to adjust to a new way of life. People with celiac disease have to be extremely careful about what they buy for lunch at school or work, what they purchase at the grocery store, what they eat at restaurants or parties, or what they grab for a snack. Eating out can be a challenge. If a person with celiac disease is in doubt about a menu item, ask the waiter or chef about ingredients and preparation, or if a gluten-free menu is available.
Gluten is also used in some medications. One should check with the pharmacist to learn whether medications used contain gluten. Since gluten is also sometimes used as an additive in unexpected products, it is important to read all labels. If the ingredients are not listed on the product label, the manufacturer of the product should provide the list upon request. With practice, screening for gluten becomes second nature.
The Gluten-free Diet: Some Examples
In 2006, the American Dietetic Association updated its recommendations for a gluten-free diet. The following chart is based on the 2006 recommendations. This list is not complete, so people with celiac disease should discuss gluten-free food choices with a dietitian or physician who specializes in celiac disease. People with celiac disease should always read food ingredient lists carefully to make sure that the food does not contain gluten.
Allowed Foods |
||
| Amaranth Arrowroot Buckwheat Cassava Corn Flax Indian rice grass |
Job’s tears Legumes Millet Nuts Potatoes Quinoa Rice |
Sago Seeds Soy Sorghum Tapioca Wild Rice Yucca |
Foods To Avoid |
||
Wheat
|
Barley Rye Triticale (a cross between wheat and rye) |
|
Other Wheat Products |
||
| Bromated flour Durum flour Enriched flour Farina |
Graham flour Phosphated flour Plain flour |
Self-rising flour Semolina White flour |
Processed Foods That May Contain Wheat, Barley, or Rye* |
||
| Bouillon cubes Brown rice syrup Chips/potato chips Candy Cold cuts, hot dogs, salami, sausage Communion wafer French fries |
Gravy Imitation fish Matzo Rice mixes Sauces |
Seasoned tortilla chips Self-basting turkey Soups Soy sauce Vegetables in sauce |
| * Most of these foods can be found gluten-free. When in doubt, check with the food manufacturer. | ||
From the following resource: Thompson T. Celiac Disease Nutrition Guide, 2nd ed. Chicago: American Dietetic Association; 2006. © American Dietetic Association. Adapted with permission. For a complete copy of the Celiac Disease Nutrition Guide, please visit www.eatright.org.
What are the complications of celiac disease?
Damage to the small intestine and the resulting nutrient absorption problems put a person with celiac disease at risk for malnutrition, anemia, and several other diseases and health problems.
- Lymphoma and adenocarcinoma are cancers that can develop in the intestine.
- Osteoporosis is a condition in which the bones become weak, brittle, and prone to breaking. Poor calcium absorption contributes to osteoporosis.
- Miscarriage and congenital malformation of the baby, such as neural tube defects, are risks for pregnant women with untreated celiac disease because of nutrient absorption problems.
- Short stature refers to being significantly under the average height. Short stature results when childhood celiac disease prevents nutrient absorption during the years when nutrition is critical to a child’s normal growth and development. Children who are diagnosed and treated before their growth stops may have a catch-up period.
How common is celiac disease?
Data on the prevalence of celiac disease is spotty. In Italy about 1 in 250 people, and in Ireland about 1 in 300 people, have celiac disease. Recent studies have shown that it may be more common in Africa, South America, and Asia than previously believed.
Until recently, celiac disease was thought to be uncommon in the United States. However, studies have shown that celiac disease is very common. Recent findings estimate about 2 million people in the United States have celiac disease, or about 1 in 133 people. Among people who have a first-degree relative diagnosed with celiac disease, as many as 1 in 22 people may have the disease.
Celiac disease could be underdiagnosed in the United States for a number of reasons including:
- Celiac symptoms can be attributed to other problems.
- Many doctors and health care providers are not knowledgeable about the disease.
- Only a small number of U.S. laboratories are experienced and skilled in testing for celiac disease.
More research is needed to learn the true prevalence of celiac disease among Americans.
Diseases Linked to Celiac Disease
People with celiac disease tend to have other autoimmune diseases. The connection between celiac disease and these diseases may be genetic. These diseases include
- thyroid disease
- systemic lupus erythematosus
- type 1 diabetes
- liver disease
- collagen vascular disease
- rheumatoid arthritis
- Sjögren’s syndrome
Dermatitis Herpetiformis
Dermatitis herpetiformis (DH) is a severe, itchy, blistering skin manifestation of celiac disease. Not all people with celiac disease develop dermatitis herpetiformis. The rash usually occurs on the elbows, knees, and buttocks. Unlike other forms of celiac disease, the range of intestinal abnormalities in DH is highly variable, from minimal to severe. Only about 20 percent of people with DH have intestinal symptoms of celiac disease.
To diagnose DH, the doctor will test the person’s blood for autoantibodies related to celiac disease and will biopsy the person’s skin. If the antibody tests are positive and the skin biopsy has the typical findings of DH, patients do not need to have an intestinal biopsy. Both the skin disease and the intestinal disease respond to a gluten-free diet and recur if gluten is added back into the diet. In addition, the rash symptoms can be controlled with medications such as dapsone (4’,4’diamino-diphenylsuphone). However, dapsone does not treat the intestinal condition and people with DH should also maintain a gluten-free diet.
Hope through Research
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) conducts and supports research on celiac disease. NIDDK-supported researchers are studying the genetic and environmental causes of celiac disease. In addition, researchers are studying the substances found in gluten that are believed to be responsible for the destruction of the immune system function, as happens in celiac disease. They are engineering enzymes designed to destroy these immunotoxic peptides. Researchers are also developing educational materials for standardized medical training to raise awareness among healthcare providers. The hope is that increased understanding and awareness will lead to earlier diagnosis and treatment of celiac disease.
Points to Remember
- People with celiac disease cannot tolerate gluten, a protein in wheat, rye, barley, and possibly oats.
- Untreated celiac disease damages the small intestine and interferes with nutrient absorption.
- Without treatment, people with celiac disease can develop complications like cancer, osteoporosis, anemia, and seizures.
- A person with celiac disease may or may not have symptoms.
- Diagnosis involves blood tests and a biopsy of the small intestine.
- Since celiac disease is hereditary, family members of a person with celiac disease may wish to be tested.
- Celiac disease is treated by eliminating all gluten from the diet. The gluten-free diet is a lifetime requirement.
- A dietitian can teach a person with celiac disease food selection, label reading, and other strategies to help manage the disease.
| The U.S. Government does not endorse or favor any specific commercial product or company. Trade, proprietary, or company names appearing in this document are used only because they are considered necessary in the context of the information provided. If a product is not mentioned, the omission does not mean or imply that the product is unsatisfactory. |
For More Information
American Dietetic Association
120 South Riverside Plaza, Suite 2000
Chicago, IL 60606–6995
Phone: 1–800–877–1600 or 312–899–0040
Fax: 312–899–4739
Email: hotline@eatright.org
Internet: www.eatright.org
Celiac Disease Foundation
13251 Ventura Boulevard, #1
Studio City, CA 91604
Phone: 818–990–2354
Fax: 818–990–2379
Email: cdf@celiac.org
Internet: www.celiac.org
Celiac Sprue Association/USA Inc.
P.O. Box 31700
Omaha, NE 68131–0700
Phone: 1–877–CSA–4CSA (272–4272)
Fax: 402–558–1347
Email: celiacs@csaceliacs.org
Internet: www.csaceliacs.org
Gluten Intolerance Group of North America
31214 124th Avenue SE
Auburn, WA 98092
Phone: 253–833–6655
Fax: 253–833–6675
Email: info@gluten.net
Internet: www.gluten.net
National Foundation for Celiac Awareness
224 South Maple Street
Ambler, PA 19002
Phone: 215–325–1306
Email: info@celiaccentral.org
Internet: www.celiaccentral.org
North American Society for Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN)
P.O. Box 6
Flourtown, PA 19031
Phone: 215–233–0808
Fax: 215–233–3918
Email: naspghan@naspghan.org
Internet: www.naspghan.org
www.cdhnf.org
Acknowledgments
This fact sheet was reviewed by Ciaran Kelly, M.D., Beth Israel Deaconess Medical Center; Mitchell Cohen, M.D., Cincinnati, Children’s Hospital Medical Center; Walter Reed Army Medical Center; National Foundation for Celiac Awareness; Celiac Disease Foundation; Celiac Sprue Association/USA Inc.; and Centers for Disease Control and Prevention staff. The gluten-free diet chart was reviewed by Alice Bast and Nancy Dickens, National Foundation for Celiac Awareness; Cynthia Kupper, R.D., C.D., Gluten Intolerance Group; and Elaine Monarch, Celiac Disease Foundation.
The Celiac Disease Awareness Campaign
To meet the need for comprehensive and current information about celiac disease, the National Digestive Diseases Information Clearinghouse (NDDIC), a service of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), launched the Celiac Disease Awareness Campaign. The Awareness Campaign is the result of the combined ideas and efforts of the professional and voluntary organizations that focus on celiac disease, along with the NIDDK, the National Institutes of Health, and the Centers for Disease Control and Prevention.
Visit www.celiac.nih.gov to learn more about the Awareness Campaign.
The National Digestive Diseases Information Clearinghouse collects resource information about digestive diseases for the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) Reference Collection. This database provides titles, abstracts, and availability information for health information and health education resources. The NIDDK Reference Collection is a service of the National Institutes of Health.
You may view the results of the automatic search on celiac disease.
If you wish to perform your own search of the database, you may access and search the NIDDK Reference Collection database online.
This publication may contain information about medications used to treat a health condition. When this publication was prepared, the NIDDK included the most current information available. Occasionally, new information about medication is released. For updates or for questions about any medications, please contact the U.S. Food and Drug Administration at 1–888–INFO–FDA (463–6332), a toll-free call, or visit their website at www.fda.gov. Consult your doctor for more information.
National Digestive Diseases Information Clearinghouse
2 Information Way
Bethesda, MD 20892–3570
Phone: 1–800–891–5389
Fax: 703–738–4929
Email: nddic@info.niddk.nih.gov
Internet: www.digestive.niddk.nih.gov
The National Digestive Diseases Information Clearinghouse (NDDIC) is a service of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). The NIDDK is part of the National Institutes of Health of the U.S. Department of Health and Human Services. Established in 1980, the Clearinghouse provides information about digestive diseases to people with digestive disorders and to their families, health care professionals, and the public. The NDDIC answers inquiries, develops and distributes publications, and works closely with professional and patient organizations and Government agencies to coordinate resources about digestive diseases.
Publications produced by the Clearinghouse are carefully reviewed by both NIDDK scientists and outside experts.
This publication is not copyrighted. The Clearinghouse encourages users of this publication to duplicate and distribute as many copies as desired.
NIH Publication No. 07–4269
August 2007